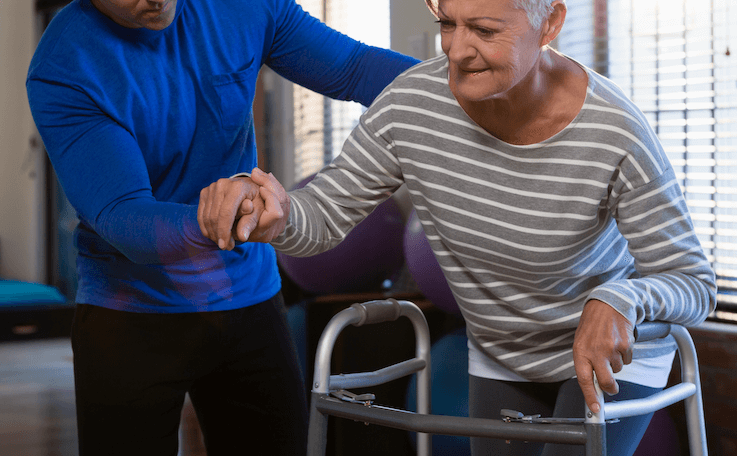About Our Practice
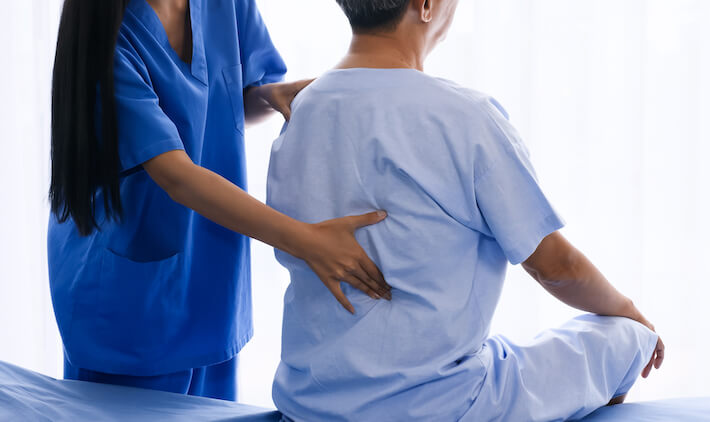
New York Spine & Sport Rehabilitation Medicine PC is dedicated to bringing patients back to their optimal level of function through a multi-disciplinary approach – providing individualized pain management solutions. Our focus is on the quality of the patient’s care with an emphasis on communication with both the patient and their referring provider to facilitate continuation of care in the patient’s home community.
Our Team
Our team of board certified, pain specializing MDs and PAs of physical medicine, rehabilitation medicine and anesthesiology background bring decades of clinical expertise to specialize in the non-operative treatment options related to spine, sports, joints, musculoskeletal, and nerve.
Our Philosophy
Our philosophy is to not only specialize in the clinical management of most acute, subacute and chronic pain conditions, but also understand why the patient is suffering from pain. Each patient at New York Spine and Sport is managed using a multidisciplinary approach, with treatment targeted at not only the condition causing the pain but also the related co-morbidities of chronic pain such as: sleep, mood, emotional disorders, lifestyle modifications, etc.
Natural history of the pain condition from simple conditions to complex pain syndromes, is explained in detail with various state of the art treatment options in consideration.
We use the latest and most advanced treatment options available to not only minimize pain, but more importantly improve physical, mental and emotional function. From traditional acupuncture, therapeutic massage, physical therapy, ergonomics, injury prevention, psychological screening, weight loss to interventional pain management techniques, we are dedicated to limiting patient suffering and improving their quality of life. In order to get to the source of pain, we utilize advanced pain interventions such as spinal cord stimulators, neuromodulator programs, kyphoplasty, percutaneous disc decompression techniques and others to get you pain-free as quickly as possible.
We believe where you get the initial treatment for pain can make all the difference. Combining active and targeted physical rehabilitation therapies, with advanced pain management interventions, is key for early recovery and favorable outcome. Inadequately treated pain can lead to the development of chronic pain syndromes with its debilitating multi-system & organ impairments.
Physical Therapy
Often the only treatment required maybe a tailored, physician directed and patient specific physical therapy program. A spine physical therapy program may include a progression, with an emphasis on pain reduction, stabilization exercises, or a gym program. Therapeutic exercises are geared to each patient’s medical condition, co morbidities, level of activity and return to physical function. Certain physical exercises, if not tailored to the condition and patient, can render treatments ineffective or even worsen the condition. Passive and prolonged physical therapy or chiropractic treatments often only relieve pain temporarily, and inadequately, while promoting further disuse, dysfunction, disability and depression (otherwise known as the 4 D Syndrome). We recommend and highly emphasize an active physical therapy program, such as soft tissue flexibility, joint mobility, abdominal and stabilization exercises, posture, body mechanics, ergonomics and if needed, modalities for spine pain.
Pain Management & Opioids
The goal of interventional pain management is to control pain, facilitate rehabilitation, and improve function. This may aid in breaking the cycle of drug dependence and disuse. Interventional pain injections/interventions are performed to direct potent medications and or heat waves to the precise source or interface of the pain. Use of steroids reduces inflammation and swelling of targeted nerve roots in the epidural or joint interface to relief pain, tingling and other symptoms. The fluoroscope allows pinpointing the pain source safely and precisely. This also allows lower steroid usage and number of procedures done per patient. By locating the source of the pain and controlling it, the body is given a chance to recover, avoid drug dependence, disability and improve overall quality of life. These injections can help diagnose and treat the source of the pain. These interventions can be initiated for patients who have significant pain scales, have used various pain medications and/or wishes to limit narcotic use or dependence. Possible benefits, side effects, complications and alternatives are discussed in detail. No contraindications should be present.
Spinal Cord Stimulator (SCS)is a neuromodulation program. If pain management blocks (such as sympathetic, epidural and or other blocks as clinically applicable), other less invasive treatments and medications are limited or short term, the patient can be a candidate for longer lasting therapy such as Spinal Cord Stimulation. The patient’s clinical examination should be consistent with chronic pain syndrome, secondary to chronic neuropathic pain from any cause – commonly from lumbar radiculopathy and post-laminectomy syndrome. There is plenty of evidence in the literature for the safety and effectiveness of SCS in these conditions. The SCS trial is intended if the patient is a candidate for the permanent implantation of SCS device. The SCS trial procedure involves insertion of temporary (trial) electrodes, and if successful in reducing pain, it is followed by a permanent implantation with minimal surgery required. This procedure is effective and may in turn reduce pain, related symptoms and improve physical and mental function.
Opioid prescription in our practice: Certain pain conditions may necessitate the use of opioids in our clinical practice, especially for severe acute or subacute (less than 4-6 weeks) pain.
Opioid medications will be tapered to the minimum, with the ultimate goal being to use only non-opioid therapeutic pain management. Patients will continue with non-opioid pain management options including non-narcotic pain medications, acupuncture, physical therapy, pain management interventions, psychological, lifestyle medications and surgical corrective surgery if needed. The patient will be explained the goals of short-term narcotic management, while natural history of the present illness is therefore taken into consideration.
Patients are explained that their narcotic use can be considered habitual. Although a patient may have a pain disease/condition, other modes of treatment should be used first – such as physical therapy, non-narcotic medications, interventional pain treatments, and psychological approach. Long term narcotic use should only be the last resort, especially for chronic pain syndrome management. The patient is explained the potential of opioid hyperalgesia, dependence, tolerance, addiction and other potential risks of chronic habitual narcotic use. We explain to our patients that the potential of tolerance can be the reason for increased use of narcotics not disease progression.
If you have been prescribed short acting opioids for more than 3 -6 months for the treatment of moderate to severe chronic pain along, with or after other treatment approaches as described above, and these treatments have been ineffective in significantly reducing pain and improving function, the pain patient is considered a candidate for long acting opioid therapy. This is undertaken after a careful review of the risks and benefits with patient.
Opioid contract, urine drug screening, and other screenings are initiated with a monthly follow up to review patients progress. Possible side effects and risks of prescribed medications are explained. Use of narcotic medications may cause side effects such as constipation, drowsiness, sedation and drug dependence are outlined. No abuse, aberrant, or adverse effects should be noted. Patients are cautioned and advised to not participate in driving motor vehicles or operating machinery or use of alcohol and other drugs interfering with motor activities. Opioid medications should always be stored in a locked cabinet.
Our Opioid contract is then reviewed, with a copy provided to patient. This documents the patient agreeing to take medications as prescribed only by our Doctors and Associates. We further outline to always keep medications safe, not abuse or misuse, use other illegal controlled substances, highlight risks and side effects including physical dependence and withdrawal condition, over dosage risks, not driving or operating machinery and submittal to a urine specimen at any time.
The Pain Medicine Questionnaire (PMQ) is also conducted as part of our opioid assessment. It helps determine how much monitoring a patient on long term opioid may require. Questions may indicate individual relative risk for developing opioid dependence and further management recommendations. Research with PMQ indicates that higher PMQ scores correlate with higher levels of substance abuse, psychopathology and physical/life functioning problems amongst patients.
Psychological Wellness for Holistic Health
NYSS” Depression Questionnaire relates to untreated and unrecognized psychopathology which can increase pain intensity, disability with functional limitations and interfere with successful rehabilitation treatments. Anxiety and depression can decrease pain thresholds/tolerances, as well as somatic amplification linked with poor treatment outcomes. Psychological testing identifies comorbidities, suggests specific treatments that may help resolve psychological risk factors, facilitates patient opioid selection by identifying compliance behavior, risks and appropriateness and may provide clues to a patient’s potential response.
The importance of weight loss and management of obesity is emphasized to help reduce the progression or reoccurrence of the above condition. Mainstay of weight management is exercise and diet control. We always explain to our patients that the above treatments are geared to control pain and speed recovery, so that ultimately desired activities/exercise yields better function.
We strongly advise patients to quit smoking, while explaining the implications of accelerated disc desiccation and degeneration with continued use, along with other medical predisposing conditions linked with its use.